As many health care providers began to develop their own set of mnemonics to remember the vast number of facts, Dr. Rather, it was referred to as many things, depending on the facility that delivered the infant. Interestingly, the term "APGAR score" was non-existent for 10 years. 3 The first scoring was only done at one minute post delivery, and later done at both the one and five minute post delivery timeframe. It was during this time that she developed the concept of a rating scale of 10 points describing the best possible condition, scoring two points each for each criteria of respiratory effort, reflex irritability, muscle tone, heart rate and color. 
Apgar reviewed the births of 2096 infants born in the Sloane Hospital for Women. Over a seven-and-a-half month time frame, Dr. Apgar was an anesthesiologist and pediatrician who sought a consistent method to evaluate newborn infants. Virginia Apgar in 1952 and introduced in 1953. It also allows consistent documentation of the newborn's condition at critical times of one and five minutes after delivery. 
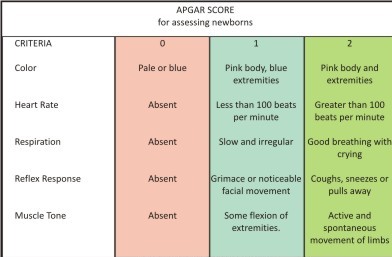
This assessment is easy to do, takes little time, and is consistent between health care providers. The APGAR score is a widely used, standard method to assess a newborn infant. 1, 2 This article will not be discussing neonatal resuscitation, but rather the APGAR scoring. Instead, resuscitation decisions are based on the clinical triad of respiration, heart rate, and color. It should be noted that the decision to begin resuscitation should not be delayed until an APGAR score is obtained. This article will discuss the APGAR scoring for a newborn assessment. Most EMS agencies can expect to deliver a baby in the field at some time or another.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
